In the United States healthcare system, millions of claims and patient records move through digital pipelines every single day. Behind this movement lies a mix of clinical documentation, billing rules, payer requirements, state-specific regulations, and automation systems. Even when everything is, designed to flow smoothly, one small inconsistency like a mismatched modifier or missing clinical detail can trigger delays, denials, and revenue loss.
This is why quality is not just a checkpoint; it is a structural foundation that supports the financial and operational health of the entire ecosystem.
Understanding the Real Challenge
Healthcare organizations today juggle rising denial rates, tighter payer scrutiny, complex regulatory demands, and pressure to maintain margins. Claims errors do not just inconvenience teams they directly affect revenue, compliance, and patient experience. Something as simple as a duplicate code or an incomplete document packet can slow down reimbursements and push accounts into the 120day aging bucket.
More importantly, leaders in healthcare, operations, and technology all experience these issues differently:
- Enterprise leaders feel the monetary impact and revenue leakage.
- Operations and RCM leaders face escalations, rework, and client dissatisfaction.
- Technology and testing leaders face system errors, workflow gaps, or automation misses.
This makes quality a cross functional priority rather than a single team’s responsibility.
The Escalating Cost of Inaccuracy
The urgency around quality becomes clearer when viewed through the lens of Revenue Cycle performance. Claims errors have a direct and measurable impact on First-Pass Yield, compliance consistency, and patient experience. Delays caused by preventable errors quickly translate into accounts moving into extended AR aging buckets, where recovery becomes increasingly difficult.
Industry data highlights the tangible financial drain of inadequate quality. The average cost to rework a single denied claim often exceeds $25, eroding already thin operating margins. Denial rates across hospitals have climbed toward 10–12%, making cash flow forecasting more volatile for leadership teams. More concerning, studies suggest that up to 90% of denials are preventable, yet they continue to recur because the underlying causes are rarely addressed upstream.
When viewed together, these metrics shift quality from a “back-office” concern to a material business risk - one that touches finance, operations, and technology equally.
The Invisible Work That Keeps Systems Running
Behind the scenes, teams responsible for supporting quality examine claims, documents, workflows, and system outputs to catch inaccuracies before they escalate. Instead of simply “checking work,” they interpret patterns, understand why issues occur, and help teams correct or prevent them.
For example, when clinical information does not match billing records, or when documentation is incomplete, they work with coding teams, providers, or process owners to make sure the corrected claim is resubmitted cleanly. The goal is not just to identify what went wrong but to make the entire process stronger.
Their work often avoids thousands even millions of dollars in potential loss. Still, this contribution stays invisible because it happens long before an issue becomes a problem.
Where Denial Insights Break Down
In organizations, denial insights stay isolated in reports and dashboards rather than forming a continuous feedback loop. Denial categories are tracked, but not consistently tied back to coding behaviour, documentation practices, or workflow design. Without closing this loop, the same denial patterns repeat, placing ongoing strain on RCM teams and slowing improvement despite awareness.
Where Most Organizations Fall Short
A common misconception in healthcare and IT is that “quality” is only an audit layer. As a result, organizations often underestimate its strategic impact.
In reality:
- When quality is reactive, problems repeat.
- When quality treated as a formality, compliance risk increases.
- When quality not integrated with operations or technology, errors spread across teams.
- When leaders do not have visibility into trends, improvement becomes guesswork.
When these gaps exist, escalations rise, rework increases, and the organization ends up spending more time fixing issues than preventing them.
Identifying the Structural Gaps
Across healthcare organizations, several recurring gaps limit the effectiveness of quality programs. Quality assurance is often disconnected from front-end workflows such as patient access and early documentation, where many issues originate. Automation and AI solutions are implemented without sufficient validation layers, resulting in errors being scaled rather than eliminated.
Additionally, QA is frequently excluded from testing and release cycles, leading to system changes that introduce avoidable disruptions. Most critically, denial analytics are not consistently translated into actionable guidance for coding and clinical documentation teams, allowing preventable denial categories to persist unchecked.
A Modern View: Quality as a Strategic Function
Healthcare is evolving rapidly, with automation, AI-assisted coding, digital transformation, and analytics becoming central to operations. But technology alone cannot solve every problem. Systems still depend on human judgment, contextual understanding, and real-world validation.
Modern quality functions blend analytics with practical insights. Instead of waiting for issues to surface, they analyse data patterns like spikes in outpatient errors or recurring issues from a particular provider and intervene early. By doing this, they shift the organization from a “corrective” mindset to a “preventive” one.
In the coming years, the focus will increasingly shift toward:
- Understanding and validating AI-driven outputs
- Strengthening automation governance
- Predicting errors before they happen
- Improving the accuracy and stability of entire workflows
- Supporting cross-team collaboration among IT, operations, and compliance
Quality becomes strategic when it helps leaders make confident, data-driven decisions.
Translating Strategy into Capability
Strategic quality delivers impact when it stabilizes workflows through sustained operational support, provides cross-system visibility across IT, operations, and compliance, and integrates directly into testing and release cycles.Moving quality upstream ensures errors are addressed before they ever enter the billing pipeline, strengthening confidence in both automation and change.
In practice, this often requires aligning workflow design, validation layers for automation and AI, and continuous operational support to ensure quality is embedded not applied after the fact.
Creating Tangible Business Impact
When quality is, integrated thoughtfully into healthcare operations, the results are visible across the organization.Claims flow faster, denials reduce, compliance becomes consistent, and provider relationships improve. Operations teams spend less time reworking and more time resolving actual problems. Leaders gain reliable insights that help them plan better and build trust with clients or payer partners.
In short: quality pays for itself, not just by preventing revenue loss, but by making the entire operation more predictable, efficient, and resilient.
Case Example Turning Quality into Cash Flow
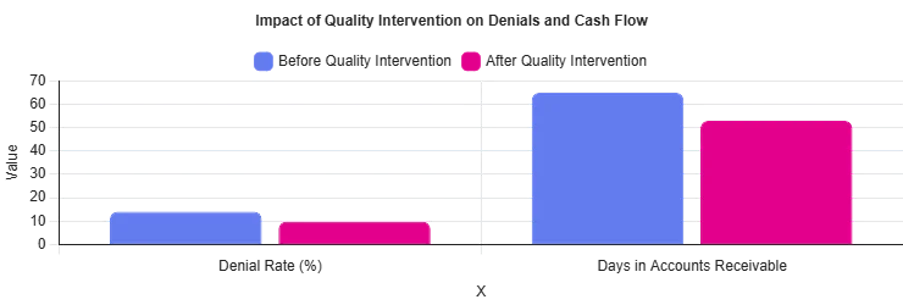
A real-world illustration of how embedding quality upstream reduced preventable denials and accelerated cash flow without adding headcount or changing core systems.
A mid-sized health system was struggling with denial rates nearing 14%. Most denials stemmed from recurring coding inconsistencies and payer edits that were identified only after claims were rejected. Quality reviews existed, but they were reactive.
By moving quality checks upstream linking denial trends back to documentation and coding, and validating changes before claims were submitted the organization saw a meaningful shift. Within six months, preventable denials dropped by close to 30%, days in AR improved by approx. two weeks, and teams reported noticeably smoother workflows as claims began flowing through the system more cleanly.
Strengthened CTA & Diagnostic Lens
As healthcare organizations prepare for the next wave of automation and AI, many are reassessing whether their current QA frameworks can truly scale without increasing risk. Two practical benchmarks often provide clarity: evaluating whether quality frameworks can support AI-driven processes at scale and conducting targeted diagnostics to identify where denial leakage originates upstream in clinical and administrative workflows.
An Invitation to Continue the Conversation
Whether you are leading healthcare operations, managing revenue cycle processes, guiding technology teams, or driving transformation initiatives, the challenges around accuracy, compliance, and financial risk are shared across the industry.
As organizations scale automation and AI, a key question is whether current quality frameworks can truly prevent denial leakage upstream and support these changes without increasing risk.
If you are evaluating this, a structured diagnostic often helps uncover where gaps exist across workflows, data, and system interactions before they impact revenue and operations.
Quality is not one team’s job it’s a coordinated effort that keeps the entire system moving with confidence.
